|
||||||||||
Upper GI endoscopy procedureDoctor ordered you a medical procedure called stomach upper gi endoscopy or esophagogastroduodenoscopy. This article will help you to understand what benefits it can bring and what you should expect before, during and after procedure. Esophagogastroduodenoscopy may be abbreviated EGD, or OGD if one uses the British spelling 'oesophago-'. It is also called upper GI endoscopy (UGIE), gastroscopy or simply endoscopy (since it is the most commonly performed type of endoscopy, the ambiguous term 'endoscopy' refers to EGD by default). Upper gi endoscopy (EGD) is one of the endoscopic study methods (inspection of internal organs with the aid of the endoscopes), that visualizes the upper part of the gastrointestinal tract up to the duodenum: the esophagus, stomach and duodenum. The patient is told not to eat for at least 4-6 hours before the procedure. Most patients tolerate the procedure with only topical anaesthesia of the oropharynx using lignocaine spray. However, some patients may need sedation and the very anxious/agitated patient may even need a general anaesthetic. Informed consent is obtained before the procedure. Side Effects and RisksA temporary, mild throat irritation sometimes occurs after the exam. Serious risks with upper GI endoscopy, however, are very uncommon. One such risk is excessive bleeding, especially with removal of a large polyp. In extremely rare instances, a perforation, or tear, in the esophagus or stomach wall can occur. These complications may require hospitalization and, rarely, surgery. Quite uncommonly, a diagnostic error or oversight may occur. Due to the mild sedation, the patient should not drive or operate machinery following the exam. For this reason, someone else should be available to drive the patient home. Endoscopy Procedure
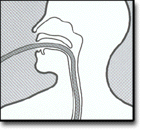
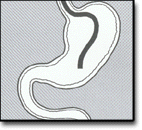
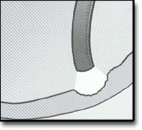
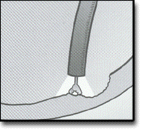
The patient lies on his/her left side with the head resting comfortably on a pillow. A mouth-guard is placed between the teeth, partly to protect the patient's teeth but more importantly to prevent the patient from biting on the very expensive endoscope. The endoscope is then passed over the tongue and into the orpharynx. This is the most uncomfortable stage for the patient. Quick and gentle manipulation under vision guides the endoscope into the esophagus. The endoscope is gradually advanced down the esophagus making note of any pathology. Excessive insufflation of the stomach is avoided at this stage. The endoscope is quickly passed through the stomach and through the pylorus to examine the first and second parts of the duodenum. Once this has been completed, the endoscope is withdrawn into the stomach and a more thorough examination is performed including a J-maneouvre. This involves bending the tip of the scope so it resembles a 'J' shape in order to examine the fundus. Any additional procedures are performed at this stage. The air in the stomach is aspirated before removing the endoscope. Still photographs can be made during the procedure and later shown to the patient to help explain any findings. In its most basic use, the endoscope is used to inspect the lining of the digestive tract. Often inspection alone is sufficient, but biopsy is a very valuable adjunct to endoscopy. Small biopsies can be made with a pincer (biopsy forceps) which is passed through the scope and allows sampling of 1 to 3 mm pieces of tissue under direct vision. The intestinal mucosa heals quickly from such biopsies. Biopsy allows the pathologist to render an opinion on later histologic
examination of the biopsy tissue with light microscopy and/or immunohistochemistry.
Biopsied material can also be tested on urease to identify Helicobacter
pylori.
More information on heartburn:Heartburn ArticlesMenopause - Doctor recommended herbal alternatives for prescription medication. |
||||||||||
                                                                               
|
||||||||||
                                                                               
|
||||||||||
|
© 2008 All Rights Reserved |
||||||||||